Según el artículo de Alexandra Sifferlin publicado en Time el 01/12/2017
First U.S. Baby Born After a Uterus Transplant
For the first time in the United States, a woman who was born without a uterus gave birth to a baby. The landmark birth took place at Baylor University Medical Center at Dallas, a part of Baylor Scott & White, TIME reports exclusively.
“We’ve been preparing for this moment for a very long time,” says Dr. Liza Johannesson, an ob-gyn and uterus transplant surgeon at Baylor. “I think everyone had tears in their eyes when the baby came out. I did for sure.” The woman and her husband asked that their identity not be revealed in order to protect their privacy
The birth took place at Baylor — the first birth in the hospital’s ongoing uterus transplant clinical trial. Women who participate in the trial have what’s called absolute uterine factor infertility (AUI), which means their uterus is nonfunctioning or nonexistent. Most of the women in the trial have a condition called Mayer-Rokitansky-Küster-Hauser (MRKH) syndrome — and have lived their entire lives under the assumption that they would never be able to be pregnant or give birth to a baby. The procedure could also work for women with other medical issues, such as certain cancers.
“We do transplants all day long,” says Dr. Giuliano Testa, the leader of the uterus transplant clinical trial at Baylor, and surgical chief of abdominal transplant for Baylor Annette C. and Harold C. Simmons Transplant Institute. “This is not the same thing. I totally underestimated what this type of transplant does for these women. What I’ve learned emotionally, I do not have the words to describe.”
The birth was a scheduled Caesarean section, and most members of the multidisciplinary clinical trial team were present. The baby was delivered healthy and screaming. “I’ve delivered a lot of babies, but this one was special,” says Dr. Robert T. Gunby Jr., the obstetrician and gynecologist who delivered the baby. “When I started my career we didn’t even have sonograms. Now we are putting in uteruses from someone else and getting a baby.”
The moment Dr. Gunby first held up the baby was emotional for many members of the medical team. “Outside my own children, this is the most excited I’ve ever been about any baby being born,” says Dr. Gregory J. McKenna, a transplant surgeon at Baylor. “I just started to cry.”
A donor’s gift
Taylor Siler, 36, a registered nurse in the Dallas area, donated her uterus to the woman who recently gave birth. Siler wasn’t always certain she wanted to have children, but she says deciding to get pregnant was one of her best decisions. “Once they lay that baby in your arms,” Siler says. “Your life changes forever.”
Siler, who has two boys aged 6 and 4, came across a news segment about Baylor’s uterus transplant program. She and her husband had already decided they were not going to have any more children, and she wanted to offer someone else a shot at motherhood. “I have family members who struggled to have babies, and it’s not fair,” says Siler. “I just think that if we can give more people that option, that’s an awesome thing.”
Siler went through extensive screening about both her physical and mental health before getting approval for the trial. Participating required surgery and about 12 weeks of recovery. Baylor says it typically takes about five hours for the wombs to be removed from the living donors, and another five to transplant.
Though she did not know the woman who received her uterus, Siler and the recipient exchanged letters on the day of the surgery, and the recipient sent Siler another letter to let her know when she was pregnant. Baylor informed Siler this week that the woman had given birth. “I’ve just been crying and getting teary thinking about it, “ says Siler, who had not yet met the new mother when she spoke to TIME. “I think about her every day and I probably will for the rest of my life.”
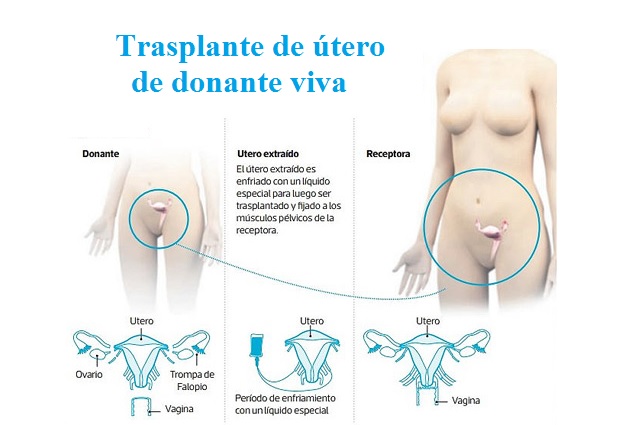
How a uterus transplant works
The women in the clinical trial are transplanted with a uterus from either a living or deceased donor. The woman who gave birth received her transplant from Siler, who was a so-called “altruistic” living donor: a stranger who volunteered to donate her uterus to a woman without one. So far, Baylor says they’ve had over 70 women express interest in donating their uterus.
Baylor will complete a total of 10 uterus transplants as part of its first trial. So far the hospital has completed eight. At least three have failed. The hospital has confirmed to Time that there is another woman in the trial who is pregnant, using a living donor uterus.
Baylor’s uterus transplant program is one of a handful to launch in the United States in recent years, and it’s the first to use both living and deceased donors. Successful uterus transplants from live donors have taken place in Sweden — a medical team at Sahlgrenska University Hospital in Gothenburg pioneered the first uterus transplant trial that resulted in eight births. This first birth at Baylor is the first to replicate that success.
Dr. Johannesson was part of the original uterus transplant team and has since moved to Texas in order to work on the Baylor program. “We were very proud of the first birth in Sweden,” she says. “But this birth is what’s going to make the field grow, because this is the first time this has been replicated anywhere else. This step is equally, if not even more, important.”
The recipients in the clinical trial are between the ages of 20 to 35, and the donors must be between ages 30 to 60. “When you donate a kidney, you do it to help someone live longer and get off dialysis,” says Dr. Testa. “For these women, they are donating an experience.”
Most of the women in the trial have moved to the Dallas area in order to undergo the procedures and the many follow up visits and tests. Once the women in the trial are transplanted with the uterus, they wait to recover and achieve menstruation, usually about four weeks from transplant. Women whose transplant is successful can then attempt in vitro fertilization (IVF). (The women in the trial have functioning ovaries that are not attached to their wombs, which is why IVF is required to get pregnant.)
Uterus transplants are expensive, with some estimates putting the cost at up to $500,000. Like other infertility treatments, it’s very rare that an insurance company would cover the procedure, which is largely viewed as elective. Baylor covered the cost of the first 10 transplants in the clinical trial, but the medical team is now seeking funding—largely through donations from institutions and private donors—in order to continue. The team says many more transplants need to be done before it could be provided as a standard treatment. “The reality is that it’s going to be very difficult for many women to afford this,” says Testa.
Renewed hope
Last year, when Baylor began the trial, Testa told TIME that the study would not be deemed a success unless the transplants resulted in a birth. Compared to other transplants that he regularly performs, like liver or kidneys, where surgeons know within minutes if the organ is working, Testa says waiting through the pregnancy after uterus transplant can feel excruciating.
“I was already nervous when my wife was pregnant, and this felt worse, like it was my pregnancy,” says Testa.
Since the procedure requires an otherwise healthy person to undergo multiple surgeries and take powerful medication, women in uterus transplant trials often say they experience comments from people asking why they don’t opt for surrogacy or adoption. “A lot of people underestimate the impact that infertility can have on a person’s wellbeing,” says Johannesson. “It can have such a profound impact.”
Baylor says they do not view uterus transplants as a replacement for other approaches like adoption or surrogacy, but as another option for women and their partners.
Baylor will continue to follow the health of the baby as part of the study. The goal is for the birth to mark the beginning of a new field of infertility treatment research, rather than be an outlier.
“For the girl who is getting the [infertility] diagnosis now, it’s not hopeless,” says Kristin Posey Wallis, a uterine transplant nurse at Baylor who works closely with women and their donors. “There’s hope.”