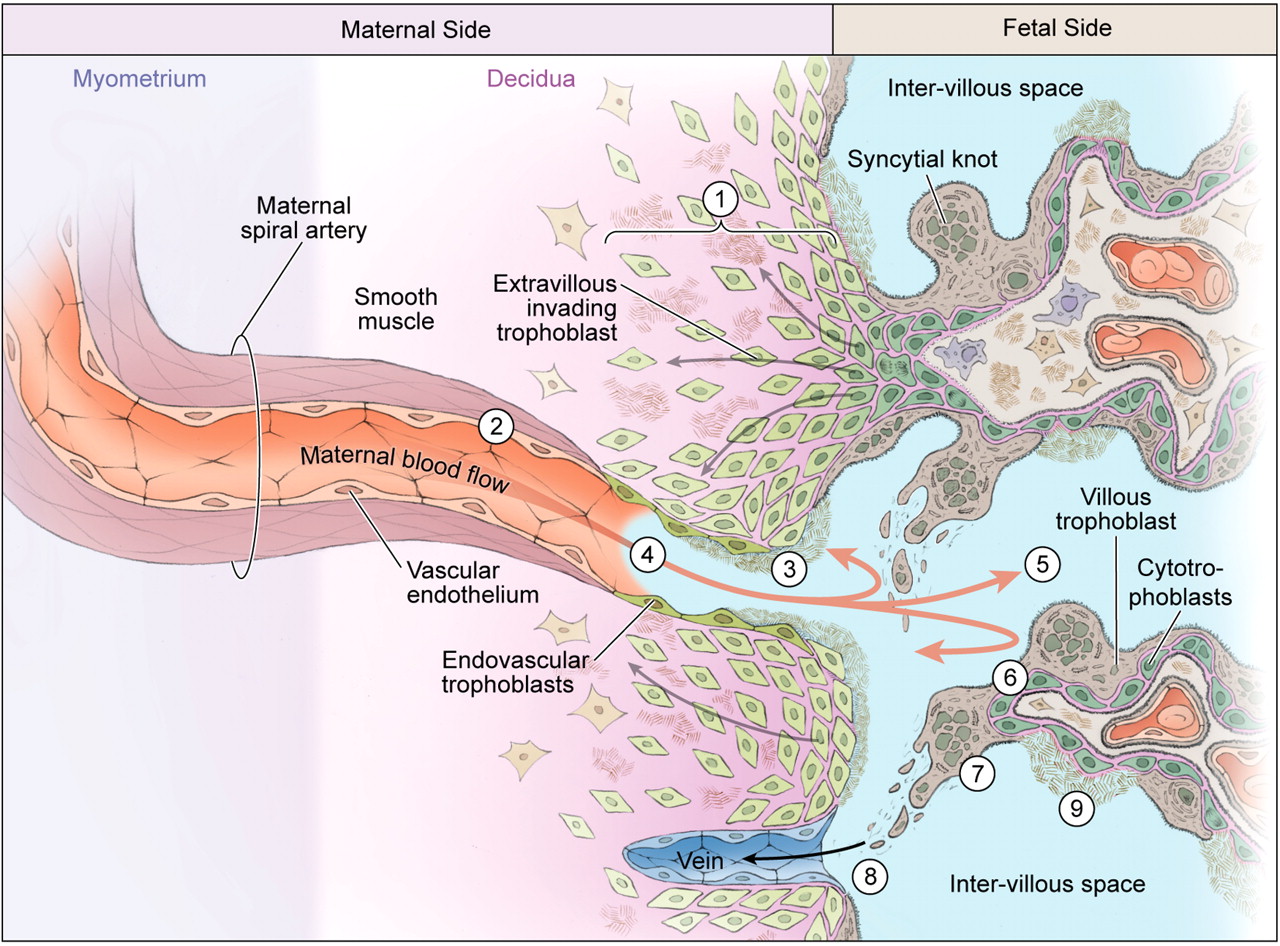
Según el artículo de Karin Winsperger publicado en human reproduction el 28/03/2017
STUDY QUESTION
Do extravillous trophoblasts (EVTs) invade non-arterial decidual vessels in healthy and pathological pregnancies?
SUMMARY ANSWER
Our results reveal that trophoblast invasion of venous and lymphatic vessels is a frequent event during the first trimester of pregnancy and is compromised in recurrent spontaneous abortion (RSA). In addition, the present data suggest that EVTs populate regional lymph nodes during pregnancy.
WHAT IS ALREADY KNOWN
Human trophoblasts remodel and invade decidual spiral arteries. In addition, a recent report demonstrates that trophoblasts contact and invade decidual veins.
STUDY DESIGN, SIZE, DURATION
Tissue samples of human first trimester deciduae basalis (n = 54, 6th–13th weeks of gestation) obtained from elective pregnancy terminations were used to study trophoblast invasion into veins and lymphatics, in comparison to arteries. Age-matched cases of idiopathic, recurrent spontaneous abortions tissue samples (n = 23) were assessed for cell numbers of EVTs in these decidual vessels. In addition, lymph nodes of four pregnant women were analysed for the presence of EVTs.
PARTICIPANTS/MATERIALS, SETTING, METHODS
Localization, frequency and EVT-mediated targeting and invasion of arterial, venous as well as lymphatic vessels were determined in first trimester decidua basalis tissue sections using immunofluorescence staining with antibodies against CD31, CD34, ephrin B2 (EFNB2), ephrin receptor B4 (EPHB4), HLA-G, podoplanin, prospero-related homeobox 1 (Prox-1), alpha-smooth muscle actin 2 (ATCTA2), von willebrand factor (vWF) and proteoglycan 2 (PRG2). Arterial, venous and lymphatic-associated EVTs were further characterized according to their position in the vascular structure and classified as intramural (im) or intraluminal (il).
MAIN RESULTS AND THE ROLE OF CHANCE
EVTs, specifically expressing PRG2, target and invade veins and lymphatics in first trimester decidua basalis since HLA-G+ trophoblast were detected in the vascular wall (intramural EVT, imEVTs) and in the lumen of these vessels (intraluminal EVT, ilEVTs). In total, 276 arteries, 793 veins and 113 lymphatics were analysed. While EVTs contact and invade arteries and veins to a similar extent we found that lymphatics are significantly less affected by EVTs (P = 0.001). Moreover, ilEVTs were detected in the lumen of venous and lymphatic vessels, whereas ilEVTs were only found occasionally in the lumen of arteries. Interestingly, RSA tissue sections contained significantly more arterial (P = 0.037), venous (P = 0.002) and lymphatic vessels (P < 0.001), compared to healthy controls. However, while RSA-associated arterial remodeling was unchanged (P = 0.39) the ratios of EVT-affected versus total number of veins (P = 0.039) and lymphatics (P < 0.001) were significantly lower in RSA compared to age-matched healthy decidual sections. Finally, HLA-G+/PRG2+/CD45-EVTs can be detected in regional lymph nodes of pregnant women diagnosed with cervical cáncer.
LIMITATIONS, REASONS FOR CAUTION
In this study, first trimester decidual tissues from elective terminations of pregnancies have been examined and used as a reference for healthy pregnancy. However, this collective may also include pregnancies which would have developed placental disorders later in gestation. Due to limitations in tissue availability our staining results for EVT-specific marker expression in regional lymph nodes of pregnant women are based on four cases only.
WIDER IMPLICATIONS OF THE FINDINGS
In this study, we propose migration of HLA-G+ cells into regional lymph nodes during pregnancy suggesting that the human EVT is capable of infiltrating maternal tissues via the blood stream. Moreover, the description of compromised EVT invasion into the venous and lymphatic vasculature in RSA may help to better understand the pathological characteristics of idiopathic recurrent pregnancy loss.
STUDY FUNDING/COMPETING INTEREST(S)
This study was supported by the Austrian Science Fund (grant P-25187-B13 to J.P. and grant P-28417-B30 to M.K.). There are no competing interests to declare.