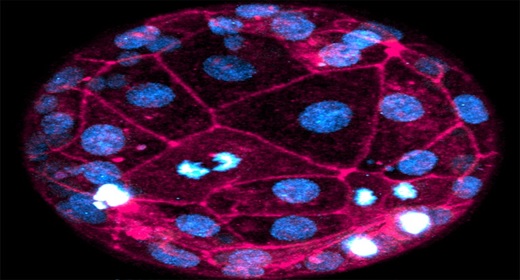
A live human embryo imaged using the fluorescent dyes SPY650-DNA (blue) and SPY555-actin (pink).Credit: Robin M. Skory, Ana Domingo-Muelas
Non-invasive imaging approach could lead to innovations in embryo screening.
According to the article of Miryam Naddaf published in Nature the 06/07/2023 and disclosed in #OKILAB
Developing human embryos imaged at highest-ever resolution
Researchers have captured the most-detailed images yet of human embryos developing in real time, using two common laboratory tools – fluorescent dyes and laser microscopes.
The technique, described in Cell on 5 July1, allows researchers to study crucial events in the first few days of development without genetically altering the embryos, which has previously restricted the use of some imaging techniques in human embryos, owing to ethical concerns.
“This is the first time we can actually image an early human embryo at the very early stages of development with cellular resolution,” says Nicolas Plachta, a cell biologist at University of Pennsylvania in Philadelphia and a co-author of the paper. “We can see single cells and how they interact with each other as they form the pre-implantation embryo.”
As well as providing a new tool for researchers, the imaging technique could lead to the development of ways to non-invasively screen embryos conceived through in vitro fertilization (IVF).
Fluorescent dyes
Researchers usually have to study human embryos using post-mortem samples, because many tools for labelling living cells involve genetically modifying them to produce fluorescent proteins.
Plachta and his colleagues developed a workaround using fluorescent dyes that can simply be added to a sample to mark particular cell structures.
The embryos used in this study were donated for research through an IVF clinic. They are at a very early stage of development — consisting of only 60 to 100 cells each — and don’t yet have any fully formed tissues or organs, says Plachta.
The researchers used SPY650-DNA, a fluorescent dye that labels genomic DNA, and SPY555-actin, which labels the protein F-actin that forms the skeleton of cells. They then visualized dozens of live embryos during the first 40 hours of development using powerful laser scanning microscopes.
“We could see those cells dividing and chromosomes segregating, and we could even capture in real time chromosome segregation defects,” says Plachta.
For example, the researchers observed that cells in the outer layer of the embryo, known as the trophectoderm, lose some of their DNA during a stage of cell replication called interphase — in which cells are replicating their DNA.
Such errors could be linked to chromosomal abnormalities such as aneuploidy, a condition that is marked by extra or missing chromosomes in the early embryo and is associated with pregnancy loss and failure of implantation.
“Knowing when aneuploidies occur allows us to get opportunities to intervene and try to correct the issue,” says Zev Williams, an obstetrician at Columbia University in New York City. The latest images reveal the first days of embryo development “with a clarity never seen before”, he adds.
Not like mice
The researchers were also able to compare key events in human embryos and mouse ones — which are often used as models to study embryonic development. They observed some important differences. For example, a process called compaction, which involves alterations in cell shape, starts at the 12-cell stage in human embryos compared with the 8-cell stage in mice; the process is also more asynchronous in human embryos, leading to variations in inner- and outer-cell formation.
“Detecting these small changes is what makes this paper so novel,” says Sade Clayton, a cell biologist at Washington University in St. Louis, Missouri. “These small differences could actually [translate to] quite large differences in terms of uterine development.”
The authors hope to build on this research by imaging human embryos for longer periods, using lower-intensity laser microscopes, and incorporating other dyes that can label different structures, such as cell membranes.
The technique might even have clinical applications one day, says Plachta. “In the future, we could use this type of live-imaging approach to follow embryos non-invasively in the clinic,” he says. This could form part of tests to determine “which embryo is likely to have the best potential” before implantation, he adds.
doi: https://doi.org/10.1038/d41586-023-02222-3
References
-
Domingo-Muelas et al. Cell 186, 1–16, https://doi.org/10.1016/j.cell.2023.06.003 (2023).